ADHD Statistics & Facts (2024): How Common Is ADHD?
Report Highlights:
- 9.3% or 5.64 million children have ADHD, affecting older children (12 to 17 years) more at 12% [24].
- 4.4% or 10.5 million American adults have ADHD. The condition affects those between 35 and 44 years more at 4.6% [14].
- ADHD is more common among boys at 12.7% and adult men at 5.4% than girls at 5.6% and adult women at 3.2% [14] [24].
- Children with longer screen time have a higher ADHD risk of 10.5% [26].
- 64% of children with ADHD also have at least one mental health problem [21].
- Only 3 in 4 American children receive ADHD treatment [21].
- 80% of adults with ADHD also suffer from at least one mental health problem [13].
- Only 10.9% of adults with ADHD receive some form of ADHD treatment [14].
- Untreated ADHD increases substance use disorder risk by 100% in teens and 58% among adults [34].
- 65% to 75% of ADHD patients show symptom improvement on stimulants like amphetamines [16].
- 75% of children with ADHD improved under behavior modification therapy [25].
- 15% of adult ADHD patients who use medical cannabis were able to wean themselves off of their ADHD medications [11].
The Centers for Disease Control and Prevention defines ADHD as one of the most common neurodevelopmental disorders. Symptoms typically begin in childhood and persist well into adulthood [22].
ADHD impacts children in different ways. However, the symptoms of ADHD or attention deficit hyperactivity disorder usually include:
- Inability to focus and pay attention, usually accompanied by fidgeting and restlessness
- Inability to control impulsive behaviors, oftentimes resulting in taking unnecessary risks
- Hyperactivity
- Difficulty making friends or getting along with people
The causes of attention deficit hyperactivity disorder include:
- Genetics
- Brain trauma and injury
- Premature delivery
- Low weight gain
- Environmental factors (exposure to chemicals, alcohol, and tobacco)
Depending on the severity of ADHD, this disorder can impact one’s day-to-day life.
How Common is ADHD?
More than 1 in 11 children have attention deficit hyperactivity disorder [24].
ADHD prevalence estimates show that nearly 1 in 22 American adults have ADHD [14].


ADHD Prevalence in Children
In the United States, childhood ADHD has a prevalence rate of 9.3%. It currently affects 5.64 million children between the ages of 3 and 17 years [24]. This data is from the 2020 National Survey of Children’s Health (NSCH) report.

Older children between 12 and 17 years have a higher prevalence rate of 13.5%. The prevalence of ADHD among younger children (4 to 11 years) is lower at 7.7% [36].
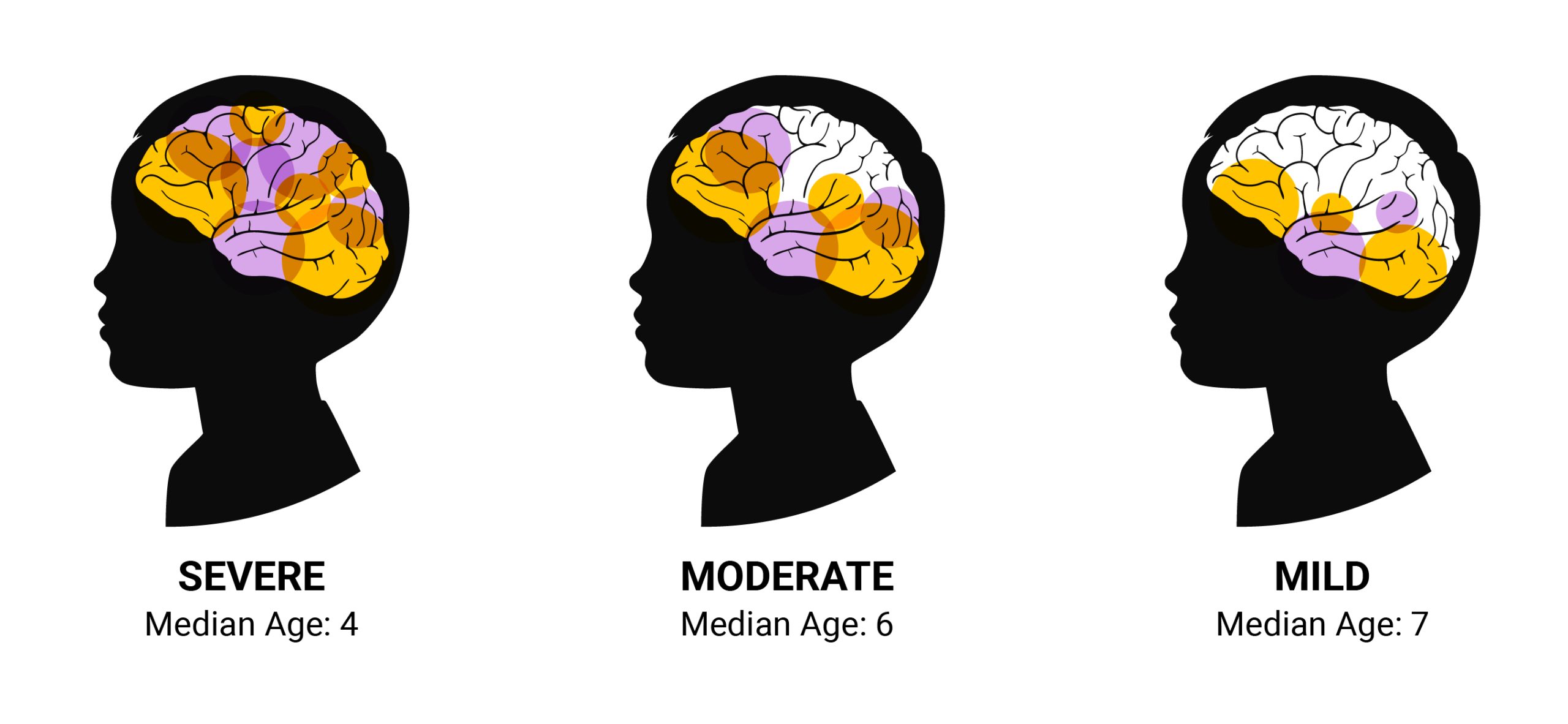
The median age of onset when ADHD symptoms start showing up in children is six years old. The younger the age of onset, the more severe ADHD symptoms that develop [23].
For severe ADHD, the median age of diagnosis is four years old. For moderate ADHD and mild ADHD, it’s six and seven years old, respectively [23].
ADHD Prevalence in Adults
Adult ADHD (18 to 44 years) has a current prevalence rate of 4.4%, affecting 10.5 million adults [14].

ADHD tends to wane as the child grows into adulthood. Hyperactivity turns into an inner restlessness that casual observers can’t easily notice.
For example, a child diagnosed with ADHD may have some difficulties keeping friends. He may also have a habit of constantly interrupting conversations. In adulthood, ADHD behavior can manifest differently. It can be constantly checking the time, forgetting to pay the bills, or divorce.
About 50% of children diagnosed with ADHD outgrow their symptoms [2].
About one-third retain their ADHD diagnosis into adulthood [23].
Is ADHD Increasing in Prevalence?
From 8.9% in 2016, childhood ADHD has increased to 9.3% in 2020 [24].
Childhood ADHD statistics show its prevalence has increased over the years [24].
Compared to childhood ADHD, we lack more research on adult ADHD. However, a study released in 2019 shed some light on adult ADHD’s increasing prevalence rate.
The 2007 to 2016 records of Kaiser Permanente Northern California were analyzed. Researchers found that the prevalence rate of adult ADHD increased to 0.96% in 2016 from 0.43% in 2007. The prevalence rate has almost doubled over a period of 10 years [6].
Why Has the Prevalence of ADHD Increased?
Several factors contribute to the increasing prevalence rate of ADHD in the country:
- More doctors recognize this neurological disorder and its symptoms.
- We’re now more aware and accepting of ADHD diagnosis.
- The stigma surrounding ADHD diagnosis has decreased.
- We now have better access to medical care. This has resulted in better methods of diagnosing the condition. It also increased the survival rates of preterm and low birth weight babies. Both of these are factors that increase ADHD risk.
- Environmental factors like high screen time and use also play a role.
Children who have more screen time have a higher risk of developing ADHD symptoms than those who don’t.
Higher Screen Time Increases ADHD Risk
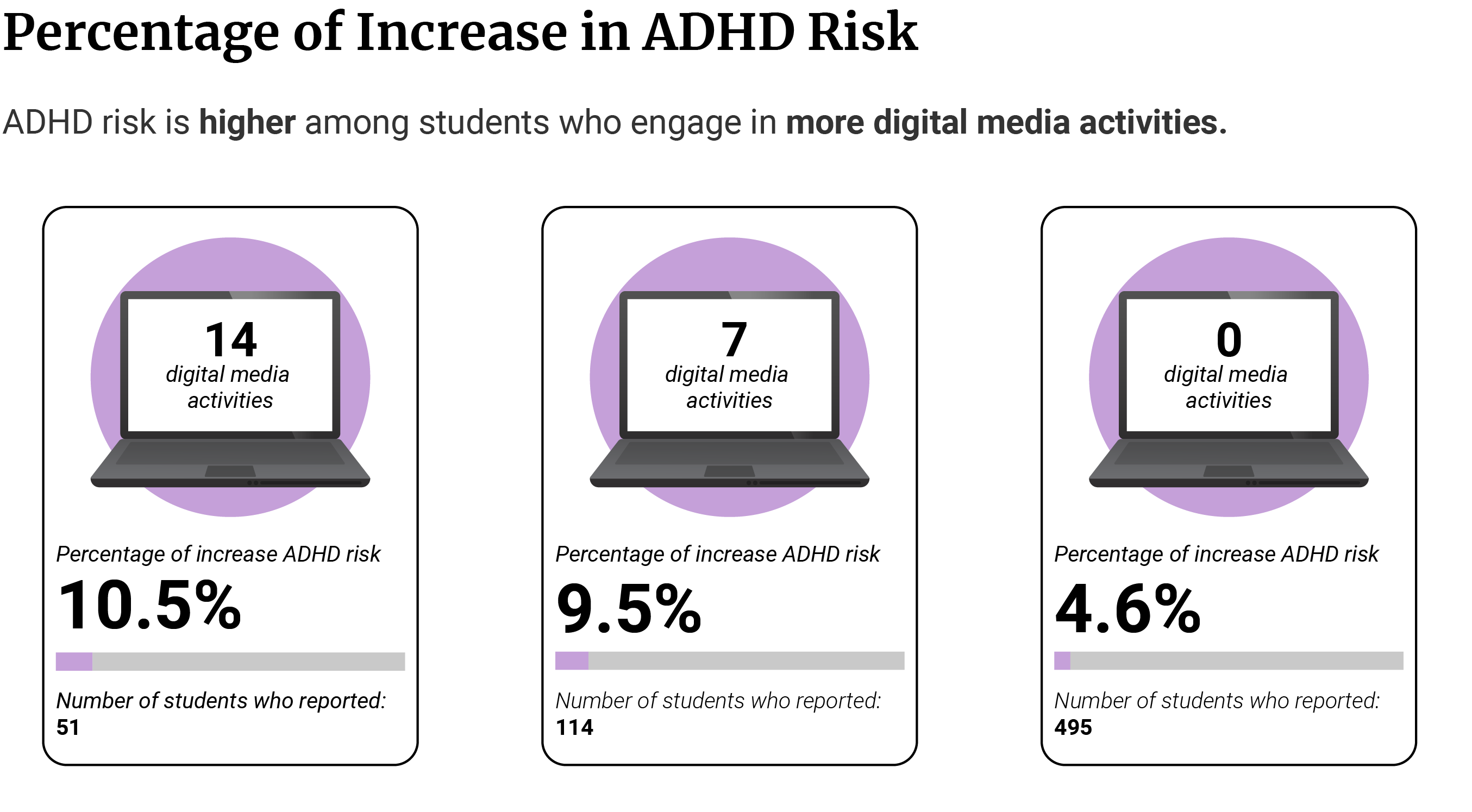
Children who engaged more in 14 digital media activities have a higher ADHD symptom prevalence of 10.5% [26].
Those who engaged in 7 out of the 14 digital media activities have an ADHD symptom prevalence of 9.5% [26].
Those who did not engage in any of the 14 digital media activities have an ADHD symptom prevalence of 4.6% [26].
Some of the digital media activities in the study included:
- Checking social media platforms
- Browsing, liking, commenting, and sharing
- Streaming movies and music
- Chatting and video-chatting
- Playing online games
- Reading blogs
- Shopping online
Of the 14 digital media activities, more than half are active on social media platforms.
54.1% check social media platforms and 52.1% text [26].
53.5% actively engage with and share other people’s posts or post their own [26].
42.9% browse and view videos online. 38.5% stream music and 25.2% stream movies [26].
33.3% play online games by themselves or with others [26].
10.1% browse or shop online [26].
Who is Most Affected by ADHD (Age Group)?
ADHD impacts adolescents aged 12 to 17 years more at 12%. 2020 NSCH data shows that 2.99 million adolescents have ADHD [24].
ADHD affects younger children aged three to five years the least at 2.3%. About 0.28 million children from this age group currently have ADHD [24].
The prevalence rate of children and adolescents diagnosed with ADHD increases with age.
As for adult ADHD, it affects more adults between 35 and 44 years at 4.6% [14]. The data came from a 2001-2003 study on American adults.
However, a 2020 global review shows adult ADHD prevalence rate decreases with age.
Persistent adult ADHD affects individuals aged 18- to 24-year-old more at 5.05%. Older people aged 60+ have a lower prevalence rate of 0.77% [28].
Who is Most Affected by ADHD (Gender and Race)?
ADHD affects boys more at 12.7% than girls at 5.6%. The NSCH’s 2020 survey shows that there are 3.96 million boys and 1.68 million girls with ADHD [24].

10.5% of non-Hispanic White children have ADHD than 2.1% of non-Hispanic Asian children. There are about 3.17 million non-Hispanic White children with ADHD. Non-Hispanic Asian children diagnosed with ADHD are about 0.06 million [24].
Adult ADHD also affects more males at 5.4% than females at 3.2% [14].


There are more non-Hispanic White adults with ADHD at 5.4% than non-Hispanic Black American adults at 1.9% [14].
ADHD Statistics in Children Receiving Treatment
Only about 3 in 4 American children receive treatment for their ADHD symptoms [21].
76.9% receive ADHD treatment. 23% do not receive any form of ADHD treatment [9].
Of those who received ADHD treatment, 30.3% received ADHD medications alone. 14.9% received behavioral treatment alone [9].
31.7% received both types of ADHD treatment [9].
9 in 10 kids diagnosed with ADHD also receive school support [21].
6 in 10 receive skills training. This includes social skills training and peer interventions [21].
How Many Children Have ADHD and Other Disorders?
64% or nearly 2 in 3 children with ADHD suffer from at least one other psychiatric disorder [21].
52% of them have behavioral or conduct problems [21].
33% also suffer from an anxiety disorder, and 17% have depression [21].
14% have a diagnosis of an autism spectrum disorder [21].
1% of the children with ADHD have Tourette syndrome [21].
ADHD Statistics in Adults Receiving Treatment
Only 10.9% of adults with ADHD receive ADHD treatment [14].
85.8% or more than 4 in 5 adults with ADHD reported no significant symptoms of ADHD [14].
Compared to their childhood disorder, their ADHD symptoms are milder. Their hyperactivity, lack of focus, inattention, or impulsive behavior becomes more controlled.
How Many Adults Have ADHD and Other Disorders?
80% of adults diagnosed with ADHD also present with other comorbid disorders [13].
5.1% to 47.1% also have bipolar disorder [13].
18.6% to 53.3% have depression, while 50% have an anxiety impairment or disorder [13].
50% have personality disorders. 25% also present with two or more types of personality disorders [13].
Personality disorders in adults with ADHD occur most among incarcerated people.
One study shows that 96% of them have an antisocial behavior personality disorder [13].
74% have borderline personality disorder. 74% also have a paranoid personality disorder [13].
Untreated ADHD Statistics
Untreated ADHD poses more lifelong risks than treated ADHD. Individuals with undiagnosed and untreated ADHD often struggle to [10]:
- Control their moods and emotions, resulting in social and relationship problems
- Finish school, resulting in employment problems. These include poor career choices and low income. Meeting deadlines or getting along with coworkers becomes difficult.
- Maintain relationships, resulting in a poor support system. This can increase the risk of dangerous behaviors. These include drug and alcohol abuse, gambling problems, and risky sexual choices. Accidents and crimes are also very common among those with untreated ADHD.
Risks of Untreated ADHD in Children and Young Adults
Among children with ADHD, those who are left untreated have a three to four times higher rate of developing substance use disorder [1].
Adolescents with untreated ADHD are more likely to self-medicate. This increases their risk of developing substance abuse by 100% [34]. The data came from a presentation sponsored by Smart Kids with Learning Disabilities.
About 58% of children with untreated ADHD also fail a school grade. One study even noted that 46% of those with untreated ADHD were suspended from school [34].
30% or nearly one-third of them fail to graduate from high school, compared to 10% of children without ADHD [34].
They also have a higher risk of unwanted pregnancy. The risk of contracting a sexually-transmitted disease also increases.
38% of them have an unwanted pregnancy or have gotten someone pregnant, compared to 4% of the same age with no ADHD [34].
17% have been infected with a sexually-transmitted disease, compared to 4% of the same age with no ADHD [34].
Risks of Untreated ADHD in Adults
Health statistics show the risks of untreated ADHD in childhood continue into adulthood.
74% of people with untreated ADHD deal with poorer outcomes than those receiving help [27].
78% of adults with untreated ADHD are more likely to develop nicotine addiction [34].
58% are also more likely to use illicit substances [34].
They’re also more prone to physical and mental disorders.
79% of adults who did not receive ADHD treatment in childhood suffer from depression. They also deal with anxiety and other chronic health problems. Among adults with no ADHD, these health issues occur in 51% of their population [34].
They’re also twice as likely to get divorced than peers of the same age [34].
The lifelong consequences of untreated ADHD in adults can also lead to crimes and jail time. 25% to 40% of those incarcerated have ADHD. Most of the cases have not been diagnosed. They have also not received any treatment for their ADHD behavior [33].
ADHD Treatment and Therapy
ADHD treatment consists of medications and behavioral treatments, including mental health counseling.
ADHD medication treatment helps stabilize neurotransmitter imbalance in the brain, which worsens ADHD. Cognitive-behavioral therapy teaches positive behaviors that can replace negative ones.
Medications for ADHD
Stimulants are the most effective ADHD drug and have a 70% to 80% responsiveness rate. 65% to 75% of the patients who use stimulants for ADHD showed significant improvement in it [16].
However, 10% to 30% of those who are taking stimulants either do not respond that well to the drug. Some have also developed adverse side effects [16].
Patients who can’t tolerate stimulant drugs are prescribed non-stimulant medications like atomoxetine. Its onset of effects may be slower than stimulants, but they’re not addictive as stimulant drugs [16].
Of the different stimulants, amphetamines produced the most benefit to ADHD. Bupropion and methylphenidate follow [7].
The most effective non-stimulants include clonidine, guanfacine, and atomoxetine [7].
Cognitive Behavioral Therapy for ADHD
75% of children receiving behavior modification therapy showed significant improvement in their symptoms. About two-thirds of them didn’t need ADHD meds after their first and second-year follow-ups [25].

Parent delivered behavior therapy is usually the first line of ADHD treatment for children less than 6 years old, says the CDC. Not only is it effective in reducing symptoms but also offers the least risk of side effects [35].
ADHD medications may also be given together with behavioral therapy. Their combination is also an effective treatment for children below the age of six. However, the benefits of behavioral therapy far outweigh stimulant drugs [35].
Among adults, cognitive-behaviorally oriented group therapy helped reduce symptoms by about 20% in 31% of the participants [15].
Mindfulness meditation training helped 30% of its participants gain a 30% reduction in their symptoms [15].
Group metacognitive therapy reduced inattentive symptoms by about 30%, compared to group supportive psychotherapy [15].
69% of adult patients receiving ADHD meds and modified cognitive therapy showed improvement. They were reclassified to being “much improved” as well as “very much improved” [15].
Their combination also helped reduce ADHD symptoms by 33% [15].
Medical Cannabis and CBD for ADHD
Depression score improved by 30% to 81% on medical cannabis. Anxiety score also increased by up to 27% [18].
Emotional regulation score improved by 22% to 78%, while inattention score improved by 7% to 30% [18].
These data came from a case study on three males with ADHD was done. It showed that adding cannabis to their ADHD treatment regimen improved their symptoms [18].
Effects of Medical Cannabis on Taking ADHD Medications
27% of the patients taking high-dose medical cannabis changed their ADHD medication regimen. 15% stopped taking their ADHD medications [11].
Of those taking lower-dose medical cannabis, 6% changed their ADHD medication regimen. 2% stopped taking their ADHD medications [11].
Note: High dose is 40 g to 70 g per month, while low dose is 20 g to 30 g per month.
Perception on Cannabis Use for ADHD
25% or 99 forum posts say cannabis helps with ADHD and improves their symptoms [19].
8% or 31 forum posts say cannabis for ADHD is more harmful than beneficial [19].
5% or 19 forum posts say cannabis is both beneficial and harmful to people with ADHD [19].
2% or 7 forum posts say it doesn't have any effects on symptoms [19].
The data came from a 2016 study that analyzed separate online forums on cannabis use for ADHD. The posts talked about the effects of cannabis on the symptoms of ADHD.
Among the people who shared their opinion or posted comments on cannabis as a medicinal agent [19]:
- 15% say that cannabis is medicinal or recommended by healthcare professionals.
- 5% say that cannabis is better than ADHD medications, while 3% say it’s not.
62 posts also mentioned the effects of cannabis on specific symptoms of ADHD [19].
74% of the posts say cannabis reduced their inattentiveness [19].
16% say it reduced their hyperactivity [19].
10% say it reduces both of these symptoms [19].
Overall, 59% of the forums advocated the therapeutic effects of cannabis for ADHD [19].
We don’t have enough detailed studies that focus on medical cannabis, especially CBD, and attention deficit hyperactivity disorder. We also lack studies on the effects of medical cannabis on children’s health. However, studies have shown that they help address many symptoms associated with ADHD. These include symptoms like anxiety and depression [32].
Cannabinoids also have anti-inflammatory properties [20]. This property can help reduce low-grade neuroinflammation, which worsens symptoms [17].
Why is There a Shortage of Adderall?
The country is currently experiencing an Adderall shortage. On October 12, 2022, the FDA confirmed the shortage [3].
The National Community Pharmacists Association (NCPA) conducted a survey on community pharmacies last August 2022. Results showed 64% of the 360 pharmacies that participated said they were having trouble getting Adderall [29].
We can expect the Adderall shortage to last for about a month or two, says CNN citing the FDA [4].
Doctors prescribe Adderall to ADHD patients. It’s a mix of amphetamine and dextroamphetamine and is considered a controlled substance. Adderall helps improve concentration and focus. It also boosts the norepinephrine and dopamine levels in the brain. This effect helps modulate behavior and mood.
The country has always had an inadequate Adderall supply since 2019 [5]. Factors that affected supply included:
- Limitations in producing this Schedule 2 controlled substance
- Limitations in distributing the drug
- An increasing number of people using Adderall
In 2009, the prescriptions filled for Adderall amounted to about $15.5 million. By 2021, it nearly tripled to $41 million, increasing by 165% in 13 years [31]. Data came from Symphony Health, the source cited by Bloomberg.
By the end of July 2022, things turned grimmer.
Labor shortages and manufacturing delays at Teva Pharmaceutical worsened the Adderall shortage [31].
Teva is the country’s primary Adderall supplier. It sold 29.8% of the country’s Adderall supply in 2021 at $565 million [31].
The popularity of telehealth services during the COVID-19 pandemic also contributed to the problem. More diagnoses necessitating the use of Adderall were made. This caused a sharp increase in the number of adults using Adderall.
In 2019, prescriptions filled for Adderall amounted to $35.3 million. This rose by 16.15% in 2021 to $41 million as the pandemic spread [31].
Adderall prescription among adults aged 22 to 44, in particular, increased by 7.4% between Q2 of 2019 and Q2 of 2020. It more than doubled to 15.1% between Q2 of 2020 and Q2 of 2021. Adderall prescription among people aged 0 to 21 and people above 45 years remained relatively stable [12].
Shortages among the other Adderall suppliers further worsened the situation.
As of October 2022, nine pharmaceutical companies reported problems supplying Adderall [30]. In addition to Teva, the list also included Mallinckrodt, Novartis, and Lannett. Together, they make up 61.3% of the country’s total Adderall sales in 2021 [31].
When Will the Adderall Shortage End?
As of the FDA’s latest update on Teva dated October 14, 2022, the country’s biggest supplier of Adderall expects to recover in November to December 2022. The report on Mallinckrodt’s SpecGx dated October 12, 2022 shows the company will have Adderall supply constraints through January 2023 [8].
If you’re short on Adderall supply, the FDA recommends working with your doctor in determining the best treatment options for your condition [3].
Final Thoughts: Are We Seeing an Increase in ADHD Diagnoses?
Attention deficit hyperactivity disorder prevalence rates are on the rise. This increase is seen not just among children but in adults as well. Factors that contribute may be increased ADHD awareness or more screen time.
Conventional ADHD medications and behavioral treatment help with disease control. However, some people also use medical cannabis. Some have even quit their ADHD medications while on medical cannabis.
ADHD isn’t just a childhood disorder. It can continue into adulthood. Untreated ADHD can cause physical problems as well as emotional and mental disorders. It can also cause social, financial, and legal problems.
If you suspect that a loved one has ADHD, seek help immediately. You may get in touch the National Alliance on Mental Illness (NAMI) at nami.org and 800-950-6264 where you’ll also find local NAMI chapters.
References
- Biederman, J. (2003). Pharmacotherapy for attention-deficit/hyperactivity disorder (ADHD) decreases the risk for substance abuse: Findings from a longitudinal follow-up of youths with and without ADHD. The Journal of Clinical Psychiatry, 64(Suppl11), 3–8. [1]
- Braaten, E. (2017). 5 things parents and teachers need to know about ADHD. Harvard Health. [2]
- Center for Drug Evaluation and Research. (2022). FDA Announces Shortage of Adderall. U.S. Food And Drug Administration. [3]
- Charles, R. (2022). Adderall users struggle amid ongoing medication shortage. CNN. [4]
- Chuck, E. (2022). FDA confirms shortage of Adderall, with delays possible until end of year. NBC News. [5]
- Chung, W., Jiang, S. F., Paksarian, D., Nikolaidis, A., Castellanos, F. X., Merikangas, K. R., & Milham, M. P. (2019). Trends in the Prevalence and Incidence of Attention-Deficit/Hyperactivity Disorder Among Adults and Children of Different Racial and Ethnic Groups. JAMA Network Open, 2(11), e1914344. [6]
- Cortese, S., Adamo, N., Del Giovane, C., Mohr-Jensen, C., Hayes, A. J., Carucci, S., Atkinson, L. Z., Tessari, L., Banaschewski, T., Coghill, D., Hollis, C., Simonoff, E., Zuddas, A., Barbui, C., Purgato, M., Steinhausen, H. C., Shokraneh, F., Xia, J., & Cipriani, A. (2018). Comparative efficacy and tolerability of medications for attention-deficit hyperactivity disorder in children, adolescents, and adults: a systematic review and network meta-analysis. The Lancet Psychiatry, 5(9), 727–738. [7]
- Current and Resolved Drug Shortages and Discontinuations Reported to FDA. (2022). U.S. Food And Drug Administration. [8]
- Danielson, M. L., Bitsko, R. H., Ghandour, R. M., Holbrook, J. R., Kogan, M. D., & Blumberg, S. J. (2018). Prevalence of Parent-Reported ADHD Diagnosis and Associated Treatment Among U.S. Children and Adolescents, 2016. Journal of Clinical Child & Adolescent Psychology, 47(2), 199–212. [9]
- Fields, L. (2021). Risks of Untreated ADHD. WebMD. [10]
- Hergenrather, J. Y., Aviram, J., Vysotski, Y., Campisi-Pinto, S., Lewitus, G. M., & Meiri, D. (2020). Cannabinoid and Terpenoid Doses are Associated with Adult ADHD Status of Medical Cannabis Patients. Rambam Maimonides Medical Journal, 11(1). [11]
- Jain, S. (2022). Sharp Uptick in Adderall Prescribing for Adults Ages 22-44 Amid COVID-19 Pandemic. Trilliant Health. [12]
- Katzman, M. A., Bilkey, T. S., Chokka, P. R., Fallu, A., & Klassen, L. J. (2017). Adult ADHD and comorbid disorders: clinical implications of a dimensional approach. BMC Psychiatry, 17(1), 302. [13]
- Kessler, R. C., Adler, L., Barkley, R., Biederman, J., Conners, C. K., Demler, O., Faraone, S. V., Greenhill, L. L., Howes, M. J., Secnik, K., Spencer, T., Ustun, T. B., Walters, E. E., & Zaslavsky, A. M. (2006). The Prevalence and Correlates of Adult ADHD in the United States: Results From the National Comorbidity Survey Replication. American Journal of Psychiatry, 163(4), 716–723. [14]
- Knouse, L. E., & Safren, S. A. (2010). Current Status of Cognitive Behavioral Therapy for Adult Attention-Deficit Hyperactivity Disorder. Psychiatric Clinics of North America, 33(3), 497–509. [15]
- Kolar, D., Keller, A., Golfinopoulos, M., Cumyn, L., Syer, C., & Hechtman, L. (2008). Treatment of adults with attention-deficit/hyperactivity disorder. Neuropsychiatric Disease and Treatment, 4(2), 389–403. [16]
- Leffa, D. T., Torres, I. L. S., & Rohde, L. A. (2018). A Review on the Role of Inflammation in Attention-Deficit/Hyperactivity Disorder. Neuroimmunomodulation, 25, 328–333. [17]
- Mansell, H., Quinn, D., Kelly, L. E., & Alcorn, J. (2022). Cannabis for the Treatment of Attention Deficit Hyperactivity Disorder: A Report of 3 Cases. Medical Cannabis and Cannabinoids, 5, 1–6. [18]
- Mitchell, J. T., Sweitzer, M. M., Tunno, A. M., Kollins, S. H., & McClernon, F. J. (2016). “I Use Weed for My ADHD”: A Qualitative Analysis of Online Forum Discussions on Cannabis Use and ADHD. PLoS ONE, 11(5), e0156614. [19]
- Nagarkatti, P., Pandey, R., Rieder, S. A., Hegde, V. L., & Nagarkatti, M. (2009). Cannabinoids as novel anti-inflammatory drugs. Future Medicinal Chemistry, 1(7), 1333–1349. [20]
- National Center on Birth Defects and Developmental Disabilities. (2020). Data and Statistics About ADHD. Centers for Disease Control and Prevention. [21]
- National Center on Birth Defects and Developmental Disabilities. (2021). What is ADHD? Centers for Disease Control and Prevention. [22]
- National Institute of Mental Health. (2021). Attention-Deficit/Hyperactivity Disorder (ADHD). National Institutes of Health. [23]
- National Survey of Children’s Health (NSCH) Interactive Data Query. (2021). Health Resources & Services Administration. [24]
- Pfiffner, L. J., & Haack, L. M. (2014). Behavior Management for School-Aged Children with ADHD. Child and Adolescent Psychiatric Clinics of North America, 23(4), 731–746. [25]
- Ra, C. K., Cho, J., Stone, M. D., De La Cerda, J., Goldenson, N. I., Moroney, E., Tung, I., Lee, S. S., & Leventhal, A. M. (2018). Association of Digital Media Use With Subsequent Symptoms of Attention-Deficit/Hyperactivity Disorder Among Adolescents. JAMA, 320(3), 255–263. [26]
- Shaw, M., Hodgkins, P., Caci, H., Young, S., Kahle, J., Woods, A. G., & Arnold, L. E. (2012). A systematic review and analysis of long-term outcomes in attention deficit hyperactivity disorder: effects of treatment and non-treatment. BMC Medicine, 10. [27]
- Song, P., Zha, M., Yang, Q., Zhang, Y., Li, X., & Rudan, I. (2021). The prevalence of adult attention-deficit hyperactivity disorder: A global systematic review and meta-analysis. Journal of Global Health, 11. [28]
- Survey: Three-Quarters of Community Pharmacies Report Staff Shortages. (2022). National Community Pharmacists Association (NCPA). [29]
- Swetlitz, I. (2022a). Adderall Shortage Expected to Continue for Months in the U.S. TIME. [30]
- Swetlitz, I. (2022b). Teva Is Facing Adderall Supply Disruptions as Demand for ADHD Drug Soars. Bloomberg. [31]
- Tambaro, S., & Bortolato, M. (2012). Cannabinoid-related Agents in the Treatment of Anxiety Disorders: Current Knowledge and Future Perspectives. Recent Patents on CNS Drug Discovery, 7(1), 25–40. [32]
- Undiagnosed Adult ADHD a High Cost for Society. (2015). Attention Deficit Disorder Association. [33]
- Untreated ADHD: Lifelong Risks. (2014). Smart Kids With Learning Disabilities. [34]
- Visser, S. N., Danielson, M. L., Wolraich, M. L., Fox, M. H., Grosse, S. D., Valle, L. A., Holbrook, J. R., Claussen, A. H., & Peacock, G. (2016). Vital Signs: National and State-Specific Patterns of Attention Deficit/Hyperactivity Disorder Treatment Among Insured Children Aged 2–5 Years — United States, 2008–2014. MMWR. Morbidity and Mortality Weekly Report, 65(17), 443–450. [35]
- Xu, G., Strathearn, L., Liu, B., Yang, B., & Bao, W. (2018). Twenty-Year Trends in Diagnosed Attention-Deficit/Hyperactivity Disorder Among US Children and Adolescents, 1997-2016. JAMA Network Open, 1(4), e181471. [36]