How Many People Have Arthritis?

Report Highlights:
- 58.5 million (24% or 1 in 4) American adults suffer from arthritis [33].
- 350 million people worldwide have arthritis [1].
- 28.2% of women and 20.1% of men in the US have arthritis [34].
- 50.4% of people over the age of 65 have arthritis [34].
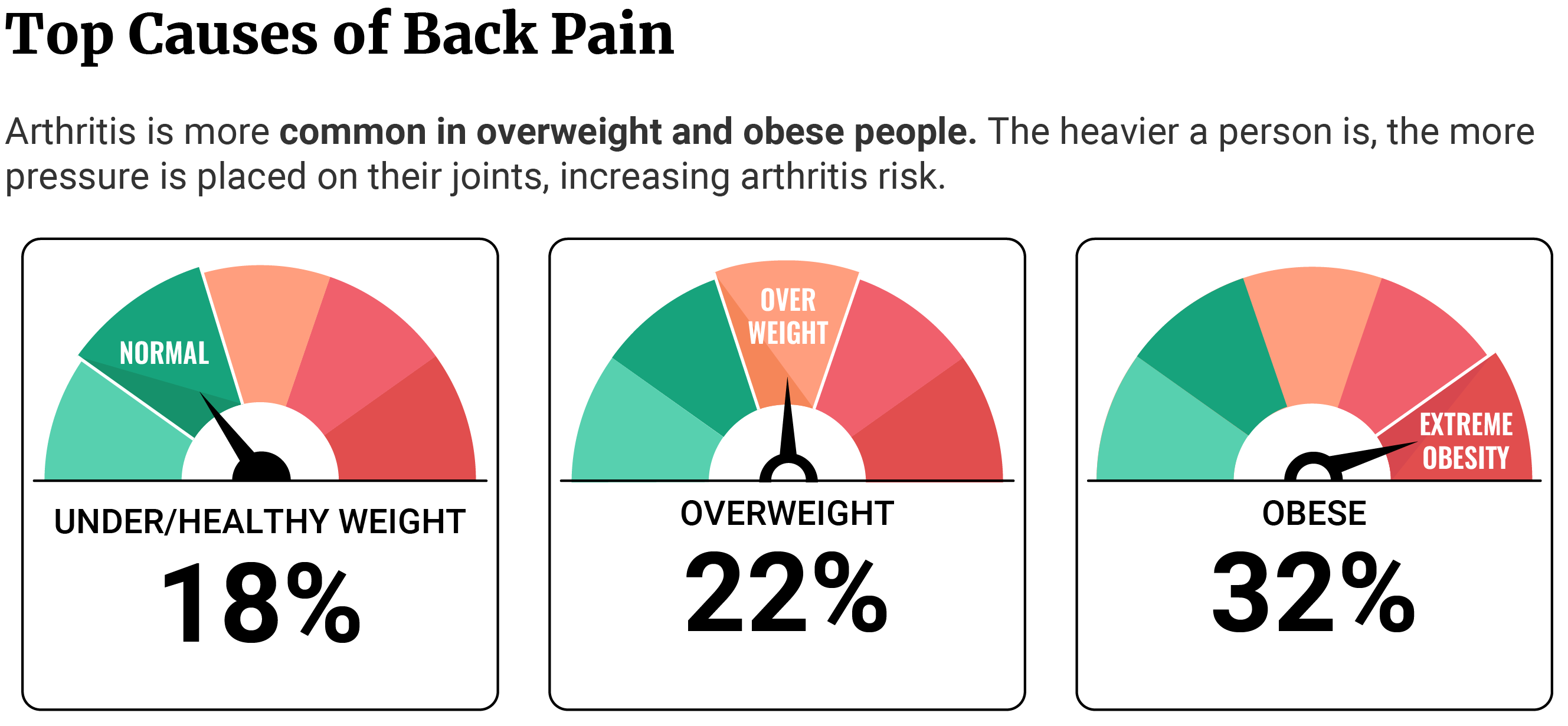
- 32% of obese and 22.2% of overweight Americans have some form of arthritis [46].
- 32.5 million American adults have osteoarthritis. It’s the most common type of arthritis [32].
- 1.3 million (0.6% to 1%) American adults suffer from rheumatoid arthritis [49].
- 14% of American adults use CBD for various reasons, and 8% of them use it for arthritis management [11].
- About 65% of osteoarthritis patients are prescribed NSAIDs [30].
- 3 out of 4 respondents in an arthritis survey say CBD improved their symptoms [38].
- Arthritis costs the US $303.5 billion yearly [33].
- Daily 20-minute and one-hour weekly exercises reduce rheumatoid arthritis risk by 35% [15].
- Losing 10 pounds of body weight slows down knee osteoarthritis progression by 50% [20].
- Smoking cessation (over 30 years) reduces seropositive rheumatoid arthritis risk by 37% [24].
- By 2040, arthritis will have affected about 78.4 million or 25.9% of American adults [36].
The Centers for Disease Control and Prevention defines arthritis as painful joint swelling. It can affect one or more joints of the body. It also affects not just older people but children as well [29].
As we scoured through arthritis studies, we found many interesting facts and statistics. Read on to know the latest arthritis statistics and facts.
What is Arthritis?
Arthritis affects 24% (58.5 million or 1 in 4) of American adults [33].
It’s also the leading cause of disability in the workplace. It costs the US $303.5 billion yearly in lost earnings and medical care costs [33].
The majority of the expenses at $164 billion go to indirect costs, which include lost earnings. About $140 billion goes to direct costs. This includes medical services, medications, and diagnostic tests [28].
Worldwide, 350 million individuals suffer from arthritis [1].
About 1 to 2 per 1,000 children worldwide also have juvenile idiopathic arthritis [7].
What are the Signs of Arthritis?
Common symptoms and signs of arthritis include:
- Painful, tender joints
- Swollen joints
- Redness of the joints
- Stiffness of the joints
- Joint range of motion problems
- Joint deformities (in worst cases)
Some people suffering from arthritis also develop anxiety and depression.
How Common are Anxiety and Depression in People with Arthritis?
22.5% or more than 1 in 5 adults suffering from arthritis have anxiety symptoms. Anxiety affects only 10.7% or nearly 1 in 9 adults with no arthritis [35].
12.1% of adults with arthritis also have depression symptoms. Only 4.7% of those with no arthritis have symptoms of depression [35].
What are the Causes of Arthritis?
Being overweight and obese can cause arthritis. The CDC reports that 22.2% of overweight and 32% of obese Americans have arthritis. Among underweight and healthy-weight Americans, only 17.6% have arthritis [46]. Heavier weight puts extreme pressure on weight-bearing joints. It damages the joints and increases arthritis risk.
With every 11 pounds gained, osteoarthritis risk also increases by 36% [37].
Obese and overweight people have a 60% likelihood of developing arthritis [37].
Obese women have about 4 times higher risk of developing osteoarthritis. Obese men also have a 5 times higher risk of developing this joint condition [37].
Inactivity also plays a role in the development of arthritis. 30.9% of those who are inactive have arthritis, compared to 27% who are insufficiently active [46].
Arthritis affects physically-active people the least. They’re also those who meet their recommended level of aerobic physical activities. Among them, only 18.8% report arthritis symptoms [46].
Age also plays a role. 50.4% of American adults over 65 years have arthritis, compared to 7.7% of those between 18 and 44 years old [34]. The risk of developing arthritis increases as we get older and our joints degenerate.
Smoking also increases arthritis risk. Current smokers have a 47% higher risk of developing rheumatoid arthritis. Former smokers also have a 22% higher risk [50]. One reason for this may be the low-grade inflammation smoking causes in the body and joints [40].
People who smoked 1 to 10 pack-years have a 26% higher risk of developing rheumatoid arthritis. The risk doubles in those with over 20-pack years [16].
Genes increase arthritis risks as well, says the American College of Rheumatology [12]:
- A family member having rheumatoid arthritis increases your risk by 0.8%. The general population has a 0.5% risk.
- One twin with rheumatoid arthritis increases the arthritis risk of the other twin by 12% to 15%. Non-identical twins have a 4% risk.
What are the Most Common Forms of Arthritis?
Osteoarthritis is the most common arthritis that affects 32.5 million adults in the US [32].
Factors that increase osteoarthritis risk include:
- Joint damage (injury, overuse, or repetitive stress on the joints)
- Age
- Genes
- Gender
- Weight
- Race
How Many People Have Osteoarthritis?
32.5 million American adults have osteoarthritis [32].
527.81 million people worldwide have osteoarthritis in 2019. This increased from 1990’s 247.51 million [23].
Osteoarthritis mostly affects weight-bearing joints like the knees.
How Many People Have Rheumatoid Arthritis in the US?
About 1.3 million, or 0.6% to 1% of American adults, have rheumatoid arthritis [49].
Worldwide, rheumatoid arthritis affects 1% of the global population [49].
Women are thrice more likely to develop rheumatoid arthritis than men [39].
40% of people with rheumatoid arthritis also experience unrelated symptoms. These include problems with the skin, eyes, heart, lungs, and nerves. Rheumatoid arthritis also affects the kidneys, bone marrow, and blood vessels [26].
It has an average point prevalence of 51 in 10,000 and a period prevalence of 56 in 10,000 people [5].
Rheumatoid arthritis is an autoimmune type of arthritis. The immune system attacks the body’s own cells. Compared to osteoarthritis, rheumatoid arthritis usually involves all joints.
How Many People Have Fibromyalgia?
4 million or 2% of the American adult population, have fibromyalgia [27].
Worldwide, 2% to 4% of the global population have fibromyalgia [19].
The cause of fibromyalgia remains unknown. However, symptoms include chronic pain and fatigue, stiffness, headaches, and sleep problems.
How Many People Have Gout?
9.2 million or 3.9% of American adults have gout [42].
Less than 1% to 6.8% of the worldwide population suffers from gout. It has an incidence rate of 0.58 to 2.89 per 1,000 person-years [14].
Gout is a type of arthritis and a complication of hyperuricemia or high blood uric acid levels. The monosodium urate crystals accumulate in and around the joints. They then irritate the joints, resulting in pain and swelling.
How Many People Have Psoriatic Arthritis or PsA?
1.5 million American adults have psoriatic arthritis. It affects about 1 in 3 people with psoriasis [22].
Worldwide, psoriatic arthritis has a 19.7% prevalence rate among patients with psoriasis. Children and adolescents have a 3.3% prevalence rate [3].
Psoriatic arthritis is a type of arthritis caused by psoriasis, a skin condition. Psoriasis causes skin hardening and scaly patches around the joints. The joints are oftentimes painful, stiff, and swollen.
How Many People Have Juvenile Arthritis or JA?
About 300,000 American children have juvenile arthritis [7].
Worldwide, juvenile arthritis affects about 3 million children and young adults [4].
Also called pediatric rheumatoid arthritis, it occurs in children under 16 years old.
How Many People Have Arthritis in the US?
58.5 million American adults have arthritis. Arthritis affects 24% or 1 in 4 adults in the US [33].
Arthritis Male vs. Female Statistics: Who is More Prone to Arthritis?
Females have a higher arthritis prevalence rate of 28.2% than males of 20.1% [34].
Other interesting arthritis male vs. female statistics worth noting:
- 60% of osteoarthritis sufferers are women [47].
- Men below 55 years old are initially more affected by osteoarthritis. After the age of 55, osteoarthritis begins to affect women more than men. The number of women with osteoarthritis soon surpasses the number of men [47].
- Women tend to experience more joint pain than men in these body locations [10]:
- Hands: Women between the ages of 50 and 60 years are 350% or 3.5 times more likely to suffer from hand osteoarthritis than men in the same age group.
- Knees: Women are 40% more likely to suffer from knee osteoarthritis than men.
- Hips: Women are 10% more likely to suffer from hip osteoarthritis than men.
- Rheumatoid arthritis affects women thrice more often than men [44].
- 90% of patients with fibromyalgia are women vs. men [48].
- Of those with rheumatoid arthritis, 58.7% of women also suffer from fibromyalgia more than men [48].
- More men suffer from gout than women at a ratio of 3:1 to 10:1 [43].
- Psoriatic arthritis affects men and women equally [17].
Arthritis Age Group: At What Age Does Arthritis Start?
Anyone can get arthritis at any age, but it seems to be highest between 30 and 65 years old [2] [6].
However, it affects older adults more than younger adults.
According to the CDC, 50.4% of American adults above 65 years old have arthritis. Only 7.7% of those between the ages of 18 and 44 years have this joint condition [34].
What Race is Most Likely to Get Arthritis?
28.4% of non-Hispanic White adults have arthritis, compared to 9% of Asians, says the CDC [34].
Whites also have the highest number of doctor-diagnosed arthritis at 41.3 million. Asians have lower doctor-diagnosed arthritis at 1.5 million [30].
Which States have the Most Arthritis?
38% of West Virginia report arthritis symptoms. It’s the state with the highest arthritis rate [34].
Alabama follows in second place with 33.3%. Kentucky comes in third place with 32.2% [34].
The District of Columbia, on the other hand, has the lowest arthritis rate. Only 16.3% of its population report arthritis symptoms [34].
California and Hawaii follow at 19.7% and 20.7%, respectively [34].
States with high arthritis prevalence rates have the highest negative health-related characteristics [34]:
- Activity limitations
- Joint pain
- Obesity
- physical inactivity
- Smoking
- High physical workload
- Socioeconomic status.
Other factors that also affect ranking include [8]:
- Access to medical care and medications
- Self-management interventions.
Is the Prevalence of Arthritis Increasing?
Around 78.4 million, or 25.9% of American adults, will be diagnosed with arthritis by a doctor by 2040 [36].
Around 52.27 million, or two-thirds of them, will be women. Men will make up one-third at 26.13 million [36].
11.4% of all adults in the US will also have arthritis-attributable activity limitations [36].
As the population grows and ages, arthritis prevalence will also increase.
Arthritis Trend in the US Through the Years
The arthritis trend in the US has remained relatively unchanged from 2015 to 2020.
24.5% of American adults have arthritis in 2020. It’s a small drop in percentage compared to 2015’s 25.3% [34].
Arthritis has always impacted women more than men. The trend remained the same from 2015 to 2020.
28.2% of women have arthritis in 2020, compared to 20.1% of men. No significant changes compared to 2015’s 28.5% of women and 20.7% of men [34].
Older adults (65+ years) have always been the age group that’s most affected by arthritis. It affects younger adults (18 to 44 years old) the least. There have been no significant changes among the age groups from 2015 to 2020 as well.
In 2020, arthritis affected 50.4% of older adults compared to 7.7% of younger adults. It decreased by a small percentage compared to 2015’s 51.6% and 8.1% [34].
How Common is Arthritis in the World?
Arthritis affects about 350 million individuals worldwide [1].
Osteoarthritis is the 5th most common cause of disability in the world. It affects 10% of people above 60 years old worldwide [7].
Rheumatoid arthritis is most common in the American region. It affects 1.25% of its population. It’s lowest in the Eastern Mediterranean region, affecting only 0.37% of its population [41].
What are the Common Drugs and Supplements for Arthritis?
Around 65% of patients with osteoarthritis receive prescriptions for NSAIDs [30].
People suffering from arthritis also take [25]:
- Steroids and corticosteroid drugs such as prednisone
- DMARDs or disease-modifying antirheumatic drugs such as leflunomide and methotrexate
- Counterirritants like capsaicin ointments
Other types of arthritis management include [25]:
- Physical therapy
- Surgery such as joint fusion, joint repair, or joint replacement
How Many Americans Use CBD for Arthritis?
14% of American adults use CBD, and 8% of them use CBD for arthritis [11].
40% of CBD users use it for pain. 4% use CBD for muscle spasms and soreness and 1% for inflammation and swelling [11].
The Arthritis Foundation surveyed 2,600 arthritic patients using CBD. It included 52% of osteoarthritis patients and 45% of rheumatoid arthritis patients [38].
Of the respondents, 94% of them use CBD for pain relief. 87% of the current CBD users also say they use CBD for arthritis symptom management [38].
63% of the respondents say they use CBD daily. 26% of them use CBD at least several times weekly [38].
The most popular CBD products come in liquid forms. 62% of them use CBD oils and tinctures. 55% also use topical CBD [38].
Does CBD Do Anything for Arthritis Symptoms?
75% or 3 out of 4 respondents reported improvement in their arthritis symptoms [38].
67% say their physical functions improved with CBD use [38].
More than 30% say CBD relieves their morning joint stiffness. CBD also helps them move around freely [38].
Is CBD Effective for Other Problems Associated with Arthritis?
71% or nearly three-fourths of the subjects say CBD helped improve their sleep quality [38].
More than 30% of them reported improvement in their fatigue symptoms [38].
41% say CBD helped improve their overall well-being. This includes emotional, mental, and physical health [38].
77% of them say CBD helped relieve their anxiety [38].
67% say CBD helped relieve their depression [38].
Frequently Asked Questions on How to Prevent Arthritis
We’ve gathered some of the frequently asked questions on preventing arthritis.
1. Can Exercise Make Arthritis Worse?
20 minutes per day of walking or biking and more than an hour of exercise per week can lower rheumatoid arthritis risk by 35% [15].
Being physically active improves function and reduces pain by about 40% [31].
72.1% of Americans with arthritis engaged in physical activities. These include walking, backpacking, and hiking. 22.8% did some muscle strengthening and aerobic exercises [18].
However, the CDC notes that only 36.2% met the guidelines for aerobic physical activity. About two-thirds of them remain aerobically inactive [18].
Physical activities help improve arthritis symptoms. They strengthen the muscles, lubricate the joints, and reduce bone loss. They also help decrease pain and swelling [9].
2. Can Losing Weight Make Arthritis Worse?
Knee osteoarthritis progression is reduced by 50% if you lose at least 10 pounds [20].
Arthritis pain decreases by 50% if you lose 10% of your body weight. Pain further decreases by 25% or more if you lose another 20% [21].
3. Does Smoking Cessation Prevent Arthritis?
Smoking cessation for over 30 years decreases the risks of seropositive rheumatoid arthritis by about 37%. The risk is higher in those who quit smoking for less than five years [24].
The longer you stop smoking, the lower your risk of developing arthritis.
4. Is a High-Fiber Diet Good for Arthritis?
15 grams of fiber daily helped reduce osteoarthritis risk by 30%, according to an Osteoarthritis Initiative study [13].
According to a Framingham study, 19 grams of fiber daily helped reduce osteoarthritis risk by 61% [13].
This data came from a research study of the two. It studied the relationship between fiber intake and osteoarthritis. Researchers found that eating high-fiber foods helps reduce osteoarthritis risk.
Foods That Worsen Arthritis
12.7% of the respondents in a rheumatoid arthritis survey said that soda with sugar worsened their symptoms [45].
12.4% said desserts, and 9.7% said beer made their symptoms worse [45].
Red meat worsened the symptoms in 7.95% of the respondents, while eggplants in 7.65% [45].
Diet soda and tomatoes also increase rheumatoid arthritis symptoms. They increased the symptoms in 7.2% and 5.25% of the respondents, respectively [45].
Less than 5% say caffeinated tea and caffeinated coffee increased their symptoms [45].
Arthritis Statistics
Arthritis affects 58.5 million Americans. It also affects more females than males. Of the different forms of arthritis, osteoarthritis is the most common. 32.5 million adults in the United States have this type of arthritis.
Conventional arthritis management controls the symptoms, but some people with arthritis find CBD also helps. Not only can it help manage their arthritis symptoms, but it improves their quality of life as well.
References
- About Arthritis and RA. (2022). Global RA Network. [1]
- Aguilar-Gaxiola, S., Loera, G., Geraghty, E. M., Ton, H., Lim, C. C., de Jonge, P., Kessler, R. C., Posada-Villa, J., Medina-Mora, M. E., Hu, C., Fiestas, F., Bruffaerts, R., Kovess-Masféty, V., Al-Hamzawi, A. O., Levinson, D., de Girolamo, G., Nakane, Y., ten Have, M., O’Neill, S., . . . Scott, K. M. (2016). Associations between DSM-IV mental disorders and subsequent onset of arthritis. Journal of Psychosomatic Research, 82, 11–16. [2]
- Alinaghi, F., Calov, M., Kristensen, L. E., Gladman, D. D., Coates, L. C., Jullien, D., Gottlieb, A. B., Gisondi, P., Wu, J. J., Thyssen, J. P., & Egeberg, A. (2019). Prevalence of psoriatic arthritis in patients with psoriasis: A systematic review and meta-analysis of observational and clinical studies. Journal of the American Academy of Dermatology, 80(1), 251–265. [3]
- Al-Mayouf, S. M., al Mutairi, M., Bouayed, K., Habjoka, S., Hadef, D., Lotfy, H. M., Scott, C., Sharif, E. M., & Tahoun, N. (2021). Epidemiology and demographics of juvenile idiopathic arthritis in Africa and Middle East. Pediatric Rheumatology, 19, 166. [4]
- Almutairi, K. B., Nossent, J. C., Preen, D. B., Keen, H. I., & Inderjeeth, C. A. (2021). The Prevalence of Rheumatoid Arthritis: A Systematic Review of Population-based Studies. The Journal of Rheumatology, 48(5), 669–676. [5]
- Arthritis. (2022). Cleveland Clinic. [6]
- Arthritis By The Numbers. (2019). Arthritis Foundation. [7]
- Barbour, K. E., Moss, S., Croft, J. B., Helmick, C. G., Theis, K. A., Brady, T. J., Murphy, L. B., Hootman, J. M., Greenlund, K. J., Lu, H., & Wang, Y. (2018). Geographic Variations in Arthritis Prevalence, Health-Related Characteristics, and Management — United States, 2015. MMWR. Surveillance Summaries, 67(4), 1–28. [8]
- Bartlett, S. (2020). Role of Exercise in Arthritis Management. Johns Hopkins Medicine. [9]
- Bracilovic, A. (2021). Why Are Women More Prone to Osteoarthritis? Veritas Health, LLC. [10]
- Brenan, M. (2019). 14% of Americans Say They Use CBD Products. Gallup, Inc. [11]
- Correia, C. S. (2018). Genetics and Rheumatic Disease. American College of Rheumatology. [12]
- Dai, Z., Niu, J., Zhang, Y., Jacques, P., & Felson, D. T. (2017). Dietary intake of fiber and risk of knee osteoarthritis in two US prospective cohorts. Annals of the Rheumatic Diseases, 76(8), 1411–1419. [13]
- Dehlin, M., Jacobsson, L., & Roddy, E. (2020). Global epidemiology of gout: prevalence, incidence, treatment patterns and risk factors. Nature Reviews Rheumatology, 16, 380–390. [14]
- di Giuseppe, D., Bottai, M., Askling, J., & Wolk, A. (2015). Physical activity and risk of rheumatoid arthritis in women: a population-based prospective study. Arthritis Research & Therapy, 17, 40. [15]
- di Giuseppe, D., Discacciati, A., Orsini, N., & Wolk, A. (2014). Cigarette smoking and risk of rheumatoid arthritis: a dose-response meta-analysis. Arthritis Research & Therapy, 16(2), R61. [16]
- Gender Differences in Psoriatic Arthritis. (2020). Johns Hopkins Medicine. [17]
- Guglielmo, D., Murphy, L. B., Theis, K. A., Boring, M. A., Helmick, C. G., Watson, K. B., Duca, L. M., Odom, E. L., Liu, Y., & Croft, J. B. (2021). Walking and Other Common Physical Activities Among Adults with Arthritis — United States, 2019. MMWR. Morbidity and Mortality Weekly Report, 70(40), 1408–1414. [18]
- Häuser, W., & Fitzcharles, M. A. (2018). Facts and myths pertaining to fibromyalgia. Dialogues in Clinical Neuroscience, 20(1), 53–62. [19]
- Here’s Why Losing Weight Is the Key to Losing Joint Pain. (2020). Cleveland Clinic. [20]
- How Fat Affects Osteoarthritis. (2020). Arthritis Foundation. [21]
- Johns Hopkins Arthritis Center. (2019). Psoriatic Arthritis. Johns Hopkins Medicine. [22]
- Klein, H. E. (2022). Osteoarthritis Is Still a Global Public Health Concern, Study Says. American Journal of Managed Care (AJMC). [23]
- Liu, X., Tedeschi, S. K., Barbhaiya, M., Leatherwood, C. L., Speyer, C. B., Lu, B., Costenbader, K. H., Karlson, E. W., & Sparks, J. A. (2019). Impact and Timing of Smoking Cessation on Reducing Risk of Rheumatoid Arthritis Among Women in the Nurses’ Health Studies. Arthritis Care & Research, 71(7), 914–924. [24]
- Mayo Foundation for Medical Education and Research (MFMER). (2021a). Arthritis. Mayo Clinic. [25]
- Mayo Foundation for Medical Education and Research (MFMER). (2021b). Rheumatoid arthritis. Mayo Clinic. [26]
- National Center for Chronic Disease Prevention and Health Promotion. (2018a). Fibromyalgia. Centers for Disease Control and Prevention. [27]
- National Center for Chronic Disease Prevention and Health Promotion. (2018b). Health and Economic Costs of Chronic Diseases. Centers for Disease Control and Prevention. [28]
- National Center for Chronic Disease Prevention and Health Promotion. (2019). Arthritis Types. [29]
- National Center for Chronic Disease Prevention and Health Promotion. (2020a). Arthritis Related Statistics. Centers for Disease Control and Prevention. [30]
- National Center for Chronic Disease Prevention and Health Promotion. (2020b). Exercise to Ease Arthritis Pain. Centers for Disease Control and Prevention. [31]
- National Center for Chronic Disease Prevention and Health Promotion. (2020c). Osteoarthritis (OA). Centers for Disease Control and Prevention. [32]
- National Center for Chronic Disease Prevention and Health Promotion. (2021a). Arthritis. Centers for Disease Control and Prevention. [33]
- National Center for Chronic Disease Prevention and Health Promotion. (2021b). Chronic Disease Indicators (CDI) Data. Centers for Disease Control and Prevention. [34]
- National Center for Chronic Disease Prevention and Health Promotion. (2021c). The Arthritis-Mental Health Connection. Centers for Disease Control and Prevention. [35]
- National Center for Chronic Disease Prevention and Health Promotion. (2022). Arthritis Data and Statistics. Centers for Disease Control and Prevention. [36]
- Obesity and Osteoarthritis. (2014). Obesity Action Coalition. [37]
- Patients Tell Us About CBD Use. (2019). Arthritis Foundation. [38]
- Rheumatoid Arthritis: Causes, Symptoms, Treatments. (2021). Arthritis Foundation. [39]
- Roh, S. (2019). Smoking as a Preventable Risk Factor for Rheumatoid Arthritis: Rationale for Smoking Cessation Treatment in Patients with Rheumatoid Arthritis. Journal of Rheumatic Diseases, 26(1), 12–19. [40]
- Rudan, I., Sidhu, S., Papana, A., Meng, S. J., Xin-Wei, Y., Wang, W., Campbell-Page, R. M., Demaio, A. R., Nair, H., Sridhar, D., Theodoratou, E., Dowman, B., Adeloye, D., Majeed, A., Car, J., Campbell, H., Wang, W., Chan, K. Y., & Global Health Epidemiology Reference Group (GHERG). (2015). Prevalence of rheumatoid arthritis in low– and middle–income countries: A systematic review and analysis. Journal of Global Health, 5(1), 010409. [41]
- Singh, G., Lingala, B., & Mithal, A. (2019). Gout and hyperuricemia in the USA: prevalence and trends. Rheumatology (Oxford, England), 58(12), 2177–2180. [42]
- Singh, J. A., & Gaffo, A. (2020). Gout epidemiology and comorbidities. Seminars in Arthritis and Rheumatism, 50(3), S11–S16. [43]
- Smith, H. R. (2022). Rheumatoid Arthritis (RA). Medscape. [44]
- Tedeschi, S. K., Frits, M., Cui, J., Zhang, Z. Z., Mahmoud, T., Iannaccone, C., Lin, T. C., Yoshida, K., Weinblatt, M. E., Shadick, N. A., & Solomon, D. H. (2017). Diet and Rheumatoid Arthritis Symptoms: Survey Results From a Rheumatoid Arthritis Registry. Arthritis Care & Research, 69(12), 1920–1925. [45]
- Theis, K. A., Murphy, L. B., Guglielmo, D., Boring, M. A., Okoro, C. A., Duca, L. M., & Helmick, C. G. (2021). Prevalence of Arthritis and Arthritis-Attributable Activity Limitation — United States, 2016–2018. MMWR. Morbidity and Mortality Weekly Report, 70(40), 1401–1407. [46]
- Why Is Arthritis In Women More Common? (2021). Summit Orthopedics. [47]
- Wolfe, F., Walitt, B., Perrot, S., Rasker, J. J., & Häuser, W. (2018). Fibromyalgia diagnosis and biased assessment: Sex, prevalence and bias. PLoS ONE, 13(9), e0203755. [48]
- Xu, Y., & Wu, Q. (2021). Prevalence Trend and Disparities in Rheumatoid Arthritis among US Adults, 2005–2018. Journal of Clinical Medicine, 10(15), 3289. [49]
- Ye, D., Mao, Y., Xu, Y., Xu, X., Xie, Z., & Wen, C. (2021). Lifestyle factors associated with incidence of rheumatoid arthritis in US adults: analysis of National Health and Nutrition Examination Survey database and meta-analysis. BMJ Open, 11(1), e038137. [50]