Does CBD Oil Help With Chronic Pancreatitis Attacks?
The pancreas is an abdominal gland located in front of the first and second lumbar vertebrae, right behind the stomach. It is responsible for digestion and metabolizing active ingredients in food and medications with external enzymes. The pancreas is made of lobules, small ducts that come from each lobe into a bigger duct. The pancreatic duct and the common bile duct connect with each other, entering the duodenum.
A healthy pancreas guarantees that metabolic functions and digestion are optimized. Any disturbance in the organ’s health may compromise these functions and lead to an array of health conditions, including pancreatitis.
Acute pancreatitis is a disease triggered by the sudden inflammation of the pancreas or the presence of gallstones trapped in the pancreatic ducts. Either of these two causes results in an obstruction of the common duct, making it impossible for the digestive enzymes to go through the intestines.
Pancreatitis can also be chronic, which is the underlying cause of Type 1 diabetes.
CBD has remarkable anti-inflammatory properties, but is it enough to relieve the symptoms of pancreatic diseases? Or should you only use it as an adjunctive treatment?
What does science say?
Let’s find out.
Does CBD Help with Pancreatitis? (Highlights)
- Research shows that CBD has anti-inflammatory effects on animals with acute pancreatitis (1).
- A 2016 study reported that CBD reduced inflammation markers in the pancreas of non-obese and diabetic rats (2).
- Another study from 2016 found that transdermal application of CBD reduced pain and inflammation in arthritic mice. Abdominal pain is one of the tell-tale symptoms of pancreatitis (3).
- In a 2020 review, CBD was found to have anti-inflammatory and antioxidant properties. Pancreatitis patients suffer from an inflamed pancreas (4).
- More human studies should be conducted on CBD’s potential therapeutic properties on pancreatitis.
CBD and Pancreatitis: What You Need to Know
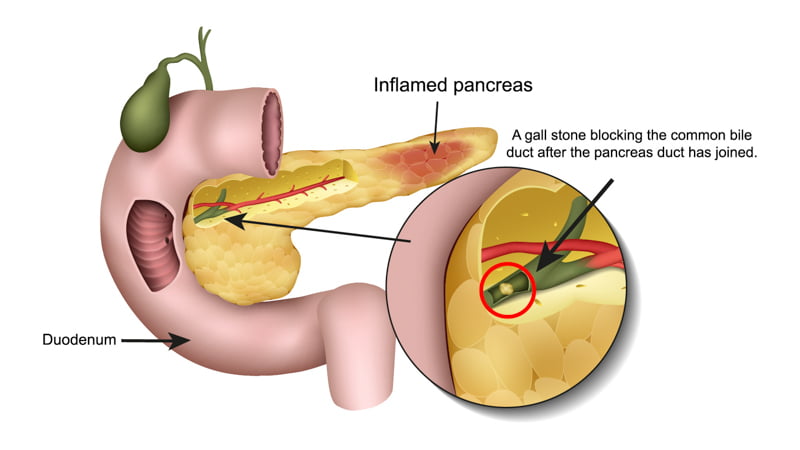
Pancreatitis treatment aims at managing pain, especially in the upper abdomen. Doctors typically prescribe painkillers for this condition.
However, conventional pain medications may cause dangerous side effects, such as brain fog, constipation, nausea, sedation, slowed breathing, and further liver damage. Prescription painkillers are also highly addictive as the user builds a tolerance to them. This, in turn, increases the risk of an overdose.
A study published in the journal Pancreas highlighted CBD’s anti-inflammatory effects in the treatment of acute pancreatitis induced in mice with cerulein. Cerulein is a decapeptide (amino acid) involved in gastrointestinal smooth muscle movements as well as in pancreatic and gastric secretions. The authors of the study also discovered that CBD improved the pathological changes in the mice and lowered the activity of the pancreatic enzymes (5).
Acute pancreatitis occurs as a result of the sudden inflammation of the pancreas. The condition may range from mild to life-threatening. However, it is typically treatable with supportive management.
A study performed on non-obese diabetic mice in 2016 found that CBD curbed inflammation markers in the pancreas of the subjects. The research team also suggested that CBD may lower the incidence of type 1 diabetes.
The pancreas plays an important role in the management of insulin. Its inability to produce sufficient amounts of insulin may lead to type 1 diabetes. Insulin is a hormone that allows the cells to process energy-producing sugar.
In a 2019 review published in the Journal of Pancreatic Cancer, the researchers investigated CBD and THC in terms of their effects on pancreatic cancer. The authors concluded that CBD and THC had antiproliferative and proapoptotic effects in pancreatic cancer models.
In other words, these cannabinoids may inhibit the growth of cancer cells and trigger their natural mechanism for programmed death. The loss of apoptotic control is one of the reasons why cancer cells can survive for long periods.
According to the review, cannabinoids may be useful as complementary therapies for pancreatic cancer. However, it recommends further research on the anti-cancer benefits of several cannabinoids, their formulations, and dosing under clinical conditions.
CBD Oil Benefits for Pancreatitis

CBD and other cannabinoids in CBD oil are derived from cannabis plants. This is the most common type of cannabinoids that can be used to treat pancreatitis. Other types include endocannabinoids (the ones produced in the body) and synthetic cannabinoids from laboratories.
Unlike THC, the other major cannabinoid, CBD doesn’t have mind-altering effects on people who take it.
Here are the most noteworthy benefits of CBD for pancreatitis.
CBD for Pancreatitis Pain
According to the current scientific literature on CBD’s potential benefits on pain-related conditions, the cannabinoid has remarkable analgesic properties.
A 2016 study reported that a topical CBD formulation reduced inflammation and pain in mice with arthritis. The mice that took 6.2 mg and 62 mg of topical CBD gels per day demonstrated reduced swelling of the joints and improved spontaneous pain markers.
The authors also mentioned that CBD didn’t have any side effects on the subjects.
In a 2020 randomized study published in the journal Current Pharmaceutical Biotechnology, the researchers analyzed CBD oil’s effects on patients suffering from peripheral neuropathy, which causes damage to nerves outside the brain and spinal cord (9).
The study found that severe neuropathic pain was reduced in the subjects that were administered CBD. Neuropathic pain is one of the side effects of chronic pancreatitis. The authors also noted that CBD was well-tolerated and might be an effective alternative to conventional painkillers prescribed for peripheral neuropathy.
A 2018 study from the journal Transplantation Proceedings evaluated CBD’s benefits for chronic pain patients who have had a kidney transplant (10).
Seven patients took 50 mg of CBD twice daily for three weeks. They slowly increased the dosage to 150 mg of CBD twice a day.
Four patients reported a positive partial response to CBD, while two patients experienced pain improvement. One patient didn’t notice any difference in pain levels.
CBD for Liver Inflammation
Inflammation is the key player in acute and chronic pancreatitis.
A 2020 review published in the journal Antioxidants pointed to CBD as a potent antioxidant and anti-inflammatory.
A 2018 study that analyzed CBD’s effects on an in vitro (outside of living organism) model of allergic contact dermatitis showed that CBD and other phytocannabinoids changed inflammatory responses by modulating cytokine production in several experimental models of inflammation. The authors noted that CBD has potent anti-inflammatory properties (12).
Cytokines are molecules that help maintain communication between the cells of the immune system. They play an essential role during immune responses, as they signal cells towards trauma sites, infection, and inflammation.
Current research suggests that oral administration of CBD might produce anti-inflammatory effects in animal models. CBD is known to help with two symptoms of inflammation — edema, and hyperalgesia.
Edema refers to swelling caused by the excessive fluid contained in the body tissues. Hyperalgesia means the increased sensitivity to pain sensations and exaggerated response to pain.
CBD for Pancreatitis-induced Nausea
Pancreatitis is often accompanied by nausea and vomiting. As reported by a study shared in the British Journal of Pharmacology, CBD may be clinically relevant in reducing these symptoms. However, the study was referring to post-chemotherapy nausea.
A 2020 study assessed the potential benefits of continuous CBD administration on rat and shrew models. The authors found that CBD reduced vomiting in the shrews (14).
The research team mentioned that CBD’s effects against nausea were similar in male and female rodents. They suggested that CBD may be effectively used in reducing nausea and preventing vomiting in patients with chronic conditions. The subjects didn’t develop tolerance to the compound.
How CBD Works to Relieve the Symptoms of Pancreatitis?
The activation of digestive enzymes, while they’re still in the pancreas, is one of the main causes of pancreatitis. This occurrence triggers inflammation as it irritates the organ’s cells.
According to a study published in the journal Proceedings of the National Academy of Sciences of the United States of America, CBD’s anti-inflammatory benefits may stem from its ability to enhance signaling of the adenosine receptor A2A (15).
The authors of the study stated that CBD blocked the uptake of adenosine and decreased serum tumor necrosis factor — the substance that causes inflammation.
As an antagonist of the A2A adenosine receptor, CBD reverses this inflammatory response, suggesting that CBD’s mechanism of improving adenosine signaling by blocking its uptake results in lowered inflammation.
CBD delays the breakdown of adenosine from the extracellular space. Adenosine is a potent anti-inflammatory molecule that regulates immune function.
CBD’s effects on the symptoms of pancreatitis are also related to its interaction with the CB2 receptors in the immune system. On top of producing anti-inflammatory effects, CBD is also able to modulate the activity of the immune system, reducing hyperactivity without shutting it down like commonly prescribed immunosuppressants.
Pros and Cons of Using CBD for Pancreatitis
The Pros:
- Studies show that CBD is a promising treatment for pancreatitis.
- CBD has an excellent safety profile. It only has a few mild side effects when consumed in large doses, including dry mouth, appetite changes, dizziness, and diarrhea.
- There is no evidence of CBD dependence on animals and humans. Therefore, the potential for substance abuse is extremely low.
The Cons:
- There are no clinical human studies that would investigate CBD’s efficacy and safety specifically for pancreatitis.
- CBD is not supported by the US Food and Drug Administration (FDA). CBD products are also unregulated, so there’s a risk of buying a mislabeled or contaminated product.
How to Use CBD for Pancreatitis?
To begin with, consider the method of administration. It should suit your lifestyle and dosage preferences aside from providing high bioavailability.
CBD is available in many different forms. The most common type of product is CBD oil. This liquid extract is suspended in an inert oil — MCT oil, hemp seed oil, or olive oil — for better absorption and easier dosing. The oil is taken under the tongue with a glass dropper. Holding it there for about 60 seconds allows for direct absorption into the bloodstream. The effects are usually felt within 15–30 minutes after administration.
If you dislike the taste of CBD oil, capsules are a good alternative. CBD capsules provide a fixed amount of cannabidiol per serving, which makes dosing easier and more convenient. Capsules are portable and easy-to-take; you just swallow them down with water. However, since they need to pass through the digestive system, the effects are delayed by 30–90 minutes.
CBD edibles, such as honey sticks and gummies are another decent option for on-the-go users. They are available in plenty of flavors and are considered the most enjoyable form of CBD. Similar to capsules, edibles need more time to kick in than oils.
If you’re looking for fast relief from your pancreatitis symptoms, CBD vape pens will be your best bet. A vape pen contains CBD E-liquid that you inhale whenever you need your dose. Inhalation delivers CBD to the bloodstream through the lung tissue. The effects usually come within minutes after puffing the liquid.
Last but not least, CBD topicals can be used to address localized discomfort, such as abdominal pain during pancreatitis. You can combine a topical formulation with one of the above formats for a multifaceted approach to treating your condition.
Choosing the Right Product
Studies show that cannabis extracts produce the best results when administered as a combination of CBD and THC. However, medical-grade CBD from marijuana isn’t federally legal, so people are turning to hemp-derived CBD oil.
Hemp-based products are categorized as health supplements, and as such, they are not regulated by any government agency. This, in turn, creates opportunities for fly-by-night companies to churn out mediocre to low-quality products at premium prices.
Here are a few steps to follow if you want to ensure the high-quality of your CBD oil:
- Check the hemp source — as dynamic bio accumulators, hemp plants absorb every substance from their environment. The best CBD oils are made from hemp that has been grown organically, in clean soil, and without pesticides. They yield CBD-rich flowers, which are the perfect source material for full-spectrum extracts.
- Opt for full-spectrum CBD — full-spectrum extracts are made from the whole plant. They contain all naturally occurring compounds in hemp, including CBD, the supportive cannabinoids, terpenes, and traces of THC. These substances help the body process CBD more efficiently due to their synergistic effects. Full-spectrum CBD is more desired than CBD isolate among users due to that mechanism.
- Look for third-party lab reports — reputable CBD companies send samples of their products to independent laboratories for testing. These laboratories analyze the potency of CBD and check for common contaminants, such as pesticides, heavy metals, mycotoxins, and solvent residue. The results should be proven with the Certificate of Analysis (CoA) displayed on the company’s site or shared on request.
CBD Dosage: How Much to Take for Pancreatitis?

When using CBD for pancreatitis, you should check with a holistic doctor experienced in cannabis use. Doing so will help you figure out the potentially effective dosage range for your situation.
The rule of thumb is to start with a low dosage and gradually increase the amount of CBD until you achieve the desired effects. Severe cases of pancreatitis may require higher-than-average doses.
Although studies haven’t yet looked at dosing for CBD in pancreatitis patients, one clinical study has found that CBD’s effects are dose-dependent. 57 participants took different doses of CBD — 150 mg, 300 mg, and 600 mg) before taking part in a simulated public speaking test.
The subjects who took 300 mg of CBD reported a significant reduction in their anxiety levels before their test. The other groups didn’t notice considerable improvements.
The research team concluded that CBD’s efficacy follows a bell-shaped dose-response pattern. However, an Israeli study from 2015 found that the pattern doesn’t apply to full-spectrum extracts, meaning that whole-plant products may be more consistent and predictable when it comes to dosage.
Summarizing the use of CBD for Pancreatitis
Pancreatitis is a debilitating condition that can affect both humans and animals. Commonly prescribed medications for this disease may have dangerous effects in pancreatitis patients, hence the popularity of CBD as a potentially effective alternative treatment.
Studies have demonstrated that CBD might not only help with the condition itself, but also with the associated symptoms. Researchers also found that CBD may alleviate pain, inflammation, and nausea — problems experienced by people with pancreatitis.
The painkilling effects of CBD appear to be bolstered when a certain amount of THC is introduced in a formulation. For this reason, you should look for products with the full spectrum of cannabinoids and terpenes.
Before taking CBD oil for pancreatitis, we encourage you to seek medical advice among professionals. The condition can be life-threatening, and a consultation with an experienced specialist will help you find the right dosage and avoid potential CBD-induced drug interactions.
Literature:
- Li, Kun et al. “Anti-inflammatory role of cannabidiol and O-1602 in cerulein-induced acute pancreatitis in mice.” Pancreas vol. 42,1 (2013): 123-9. doi:10.1097/MPA.0b013e318259f6f0
- Lehmann, Christian et al. “Experimental cannabidiol treatment reduces early pancreatic inflammation in type 1 diabetes.” Clinical hemorheology and microcirculation vol. 64,4 (2016): 655-662. doi:10.3233/CH-168021
- Hammell, D C et al. “Transdermal cannabidiol reduces inflammation and pain-related behaviors in a rat model of arthritis.” European journal of pain (London, England)vol. 20,6 (2016): 936-48. doi:10.1002/ejp.818
- Atalay, Sinemyiz et al. “Antioxidative and Anti-Inflammatory Properties of Cannabidiol.” Antioxidants (Basel, Switzerland) vol. 9,1 21. 25 Dec. 2019, doi:10.3390/antiox9010021
- Sharafi, Golnaz et al. “Potential Use of Cannabinoids for the Treatment of Pancreatic Cancer.” Journal of pancreatic cancer vol. 5,1 1-7. 25 Jan. 2019, doi:10.1089/pan can.2018.0019
- Lehmann, C. op. cit.
- Sharafi, Golnaz et al. “Potential Use of Cannabinoids for the Treatment of Pancreatic Cancer.” Journal of pancreatic cancer vol. 5,1 1-7. 25 Jan. 2019, doi:10.1089/pan can.2018.0019
- Hammell, D C. op. cit.
- Sharafi, Golnaz et al. “Potential Use of Cannabinoids for the Treatment of Pancreatic Cancer.” Journal of pancreatic cancer vol. 5,1 1-7. 25 Jan. 2019, doi:10.1089/pan can.2018.0019
- Xu, Dixon H et al. “The Effectiveness of Topical Cannabidiol Oil in Symptomatic Relief of Peripheral Neuropathy of the Lower Extremities.” Current pharmaceutical biotechnology vol. 21,5 (2020): 390-402. doi:10.2174/1389201020666191202111534
- Shafari, G. op. Cit.
- Cuñetti, L et al. “Chronic Pain Treatment With Cannabidiol in Kidney Transplant Patients in Uruguay.” Transplantation proceedings vol. 50,2 (2018): 461-464. doi:10.1016/j.transproceed.2017.12.042
- Petrosino, Stefania et al. “Anti-inflammatory Properties of Cannabidiol, a Nonpsychotropic Cannabinoid, in Experimental Allergic Contact Dermatitis.” The Journal of pharmacology and experimental therapeutics vol. 365,3 (2018): 652-663. doi:10.1124/jpet.117.244368
- Rock, Erin M et al. “Evaluation of repeated or acute treatment with cannabidiol (CBD), cannabidiol acid (CBDA) or CBDA methyl ester (HU-580) on nausea and/or vomiting in rats and shrews.” Psychopharmacology vol. 237,9 (2020): 2621-2631. doi:10.1007/s00213-020-05559-z
- Carrier, Erica J et al. “Inhibition of an equilibrative nucleoside transporter by cannabidiol: a mechanism of cannabinoid immunosuppression.” Proceedings of the National Academy of Sciences of the United States of America vol. 103,20 (2006): 7895-900. doi:10.1073/pnas.0511232103